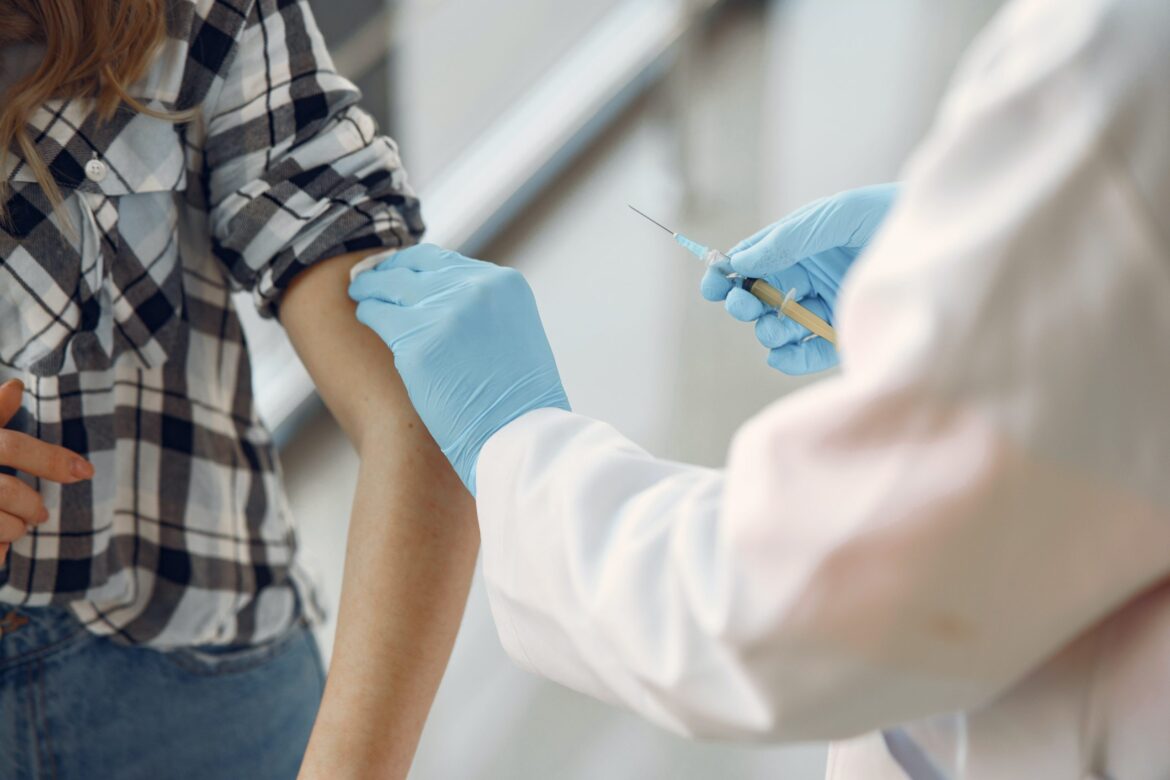
The integrated research organization “Javara” announced that it will invite the elderly, age 60 and older, in three southern states in the U.S to participate in the phase 3 RENOIR developed by Pfizer to protect them from the respiratory syncytial virus (RSV) and confirm its safety and efficacy in preventing moderate to severe lower respiratory tract illness associated with RSV.

Winston-Salem, NC (Merxwire) – “Javara” recently announced that it will invite the elder adult, age 60 and older, in the communities of Texas, Georgia, and North Carolina in the southern United States to participate in clinical trials of vaccines against RSV. This trial will recruit 30,000 participants around the world who are healthy or have stable chronic conditions to receive the new RSV vaccine or placebo. The purpose of this test is mainly to reduce the risk of RSV virus in the elderly through vaccination.
RSV is a single-stranded RNA virus that usually begins to spread in late autumn, with winter as the main infectious period, which can cause respiratory infections of all ages. The incubation period after infection is extremely short, only 2 to 8 days. The most frightening part of this virus is that its disease progressed quite rapidly. It may only take 2 to 3 days to develop from mild cold symptoms or fever to severe respiratory distress syndrome, pneumonia, or bronchitis. At present, no drug could treat the RSV virus directly, and no vaccine can prevent RSV for a long time. Therefore, many pharmaceutical companies are researching vaccines that can prevent RSV. The vaccine for the third phase of clinical trials is “RENOIR” developed by Pfizer. If approved, it would be the first vaccine available for the prevention of RSV and safely reduce the moderate to severe illnesses by RSV and the serious health threat for older adults.
The RSV virus had a rare increase in infections in the United States this summer, especially in the southern United States. The number of inpatients and confirmed cases of infants and children reported by the hospitals was higher than the average for the same period in previous years. Dr. Hossein Sadeghi, associate professor of pediatrics at Columbia University College of Physicians and Surgeons, believed that is because the COVID-19 had slowed down this year. People took off their masks, neglected to clean their hands, and started traveling after being vaccinated. Therefore, the RSV virus spreads more quickly.
Premature babies, infants with low immunity, and the elderly over 65 are the main targets of the RSV virus, and they are also a high-risk group for severe lower respiratory tract infections. Each year in the U.S., more than 177,000 adults, age 65 and over, are hospitalized due to RSV, with an estimated 14,000 of those cases proving fatal. Therefore, we have to pay attention to the cluster infection of the elderly and young children, such as homes of the elders, long-term care institutions, kindergartens, and postpartum care centers that are more popular in Asia.

But whether vaccination is the cure to the disease, there is still no definite answer. Scientists have studied the psychological factors of people who are in doubt about vaccination for a long time, and deduced the well-known “5C” theory:
- Confidence: Do people have confidence in the efficacy and safety of the vaccine? Do people have confidence in the vaccine manufacturer and the policy of the government? These all affect people’s willingness to take the vaccination.
- Complacency: Does this disease pose a threat to my health? If I am healthy now, maybe I don’t need to be vaccinated.
- Calculation: Comparing the advantages and disadvantages of vaccination and non-vaccination by collecting a large amount of data.
- Constraints or convenience: Are there any restrictions on vaccination, and is it easy and convenient to go for vaccination? The difficulty of vaccination affects people’s thinking.
- Collective responsibility: Regard vaccination as a social responsibility, and consider whether to vaccinate to protect other people.
In addition to the “5C” theory, recent studies conducted by Oxford University found that about 10% of people are unwilling to get vaccinated because they are afraid of injections.
As COVID-19 spreads across the world, most governments in various countries use “vaccination” as a preventive policy, and they are also engaged in a battle with people who are unwilling to vaccinate. According to survey data from the International Monetary Fund, the lower proportion of the population unwilling to receive the vaccine is the U.K, about ten to twenty percent, and the higher proportion is Japan and France, about fifty to sixty percent. How to overcome the people’s psychological barriers and how to persuade the people to accept the vaccine with scientific rationality will still be a difficult topic for governments of all countries.